Introduction
Milia skin, those tiny, pearly white bumps that can pop up on your face and leave you scratching your head in confusion. What are they, and why do they appear? Don’t worry; you’re not alone in your quest for answers. In this comprehensive guide, we’ll exploring their causes, treatment options, and prevention strategies. So, discover how to keep your skin smooth and clear!
What are Milia?
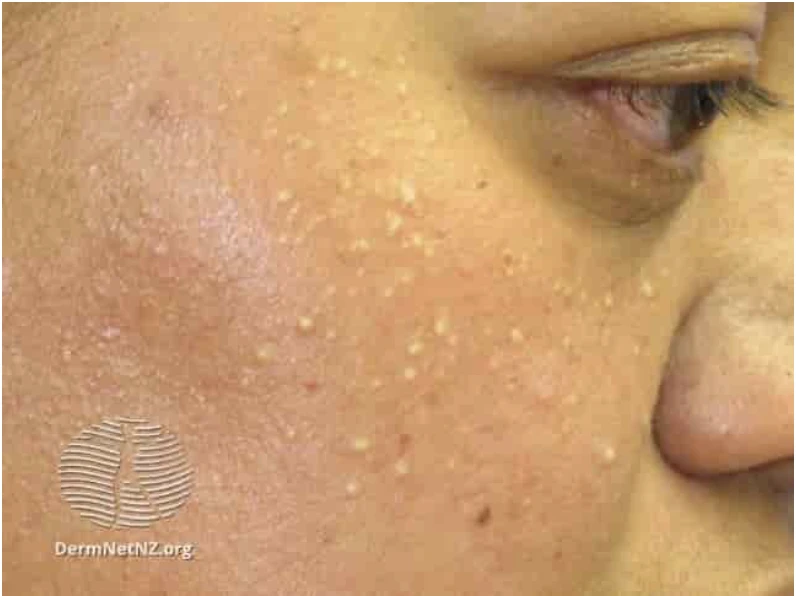
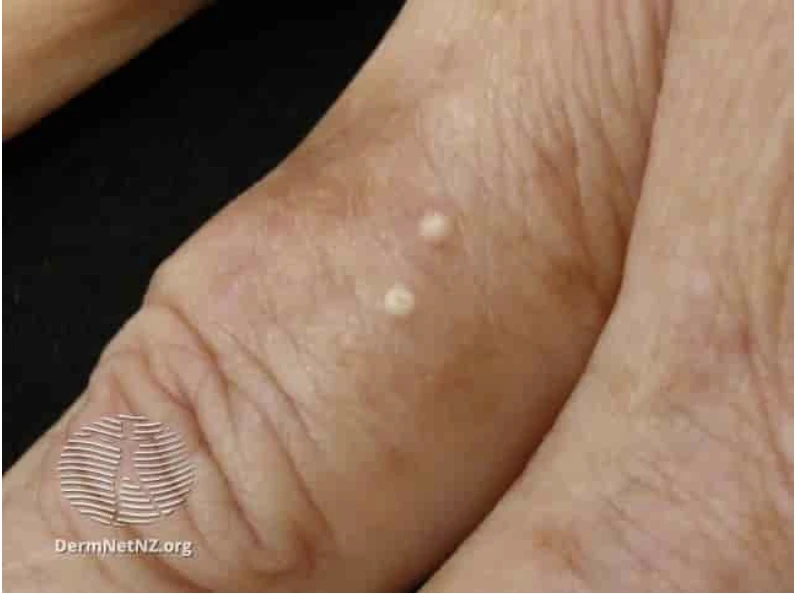
Milia (singular: milium) are small, harmless cysts that typically appear as tiny white or yellowish bumps on the skin’s surface. They can show up on various parts of your body, but they’re most commonly found on the face, particularly around the eyes, nose, and cheeks. it might resemble whiteheads, but they’re quite different in terms of their formation and content.

Types of Milia
Before we jump into prevention and healthcare provider consultations, let’s get to know the various types of milia. Understanding the type is the first step in managing it effectively.
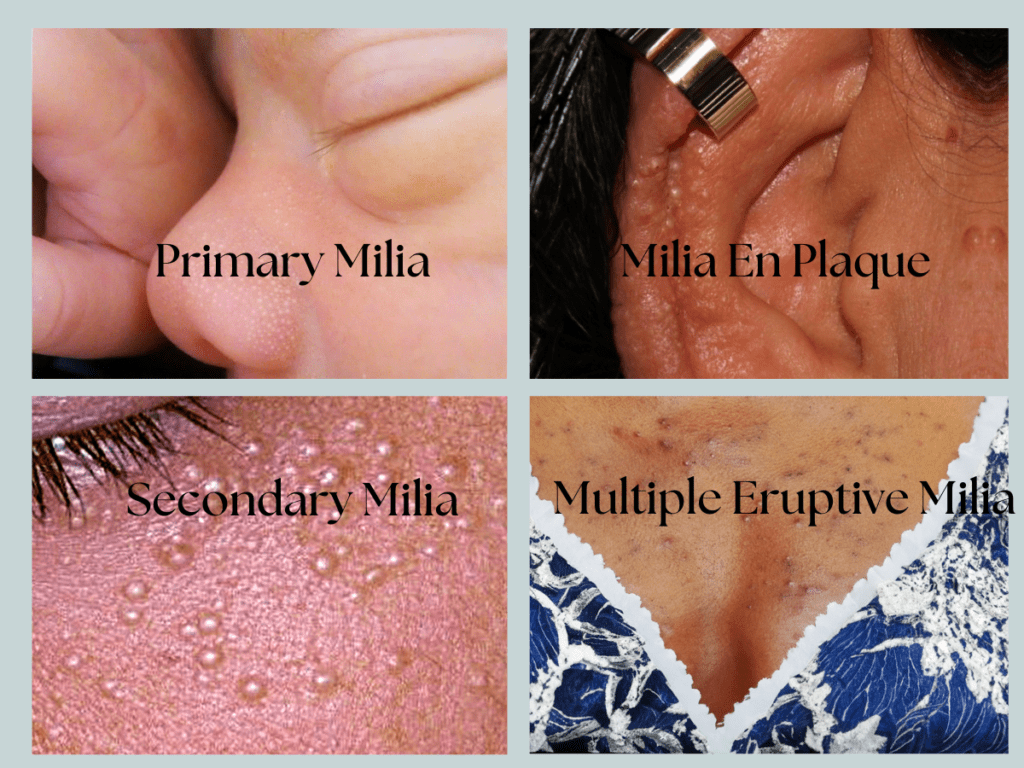
1. Primary Milia
It is also known as “neonatal milia,” typically appear in infants. These tiny, pearly white or yellowish bumps commonly occur on the nose and cheeks. They’re caused by trapped skin flakes and are usually harmless, clearing up on their own within a few weeks.
2. Secondary Milia
Secondary milia are a bit different. These can affect individuals of any age, and they arise as a result of skin damage. Common causes include:
- Blistering from a burn
- Trauma to the skin
- Long-term use of heavy cosmetics
- Certain topical medications
It can be more persistent and may require treatment to resolve.
3. Milia En Plaque
It is a rarer form of milia. It presents as a group of milia that cluster together in an inflamed patch. This type is often associated with autoimmune skin disorders and typically requires medical attention.
4. Multiple Eruptive Milia
They are characterised by crops of milia that suddenly appear in clusters, often on the face, upper arms, or upper trunk. While the cause is not always clear, this type may be linked to genetic factors. They can resolve on their own but might take several months.

What Causes Milia Skin?
Understanding the underlying causes of milia is crucial for effective prevention and treatment. Several factors can contribute to the development of these tiny cysts, including:

1. Dead Skin Cells Buildup
It occur when dead skin cells become trapped under the skin’s surface. This can happen for various reasons, such as inadequate exfoliation or a sluggish skin turnover process. When these dead cells aren’t shed properly, they can accumulate and form milia.
2. Injury or Trauma
Sometimes, it can form in response to skin injuries, burns, or blistering. The damaged skin traps keratin, a protein found in hair and skin, beneath the surface. This trapped keratin can then develop into milia over time.
3. Topical Products
Certain skincare products, especially those rich in heavy creams or oils, can contribute to development. These products may contain ingredients that clog pores and hinder the natural shedding of dead skin cells. When the shedding process is disrupted, milia can form.
4. Sun Damage
Prolonged exposure to the sun’s harmful UV rays can lead to milia. Sun damage can thicken the skin, making it more difficult for dead skin cells to shed properly. This can create a favourable environment for milia to develop.
5. Genetics
In some cases, it may have a genetic component, making certain individuals more predisposed to developing these cysts. If milia run in your family, you may be more likely to experience them, even with proper skincare
How to Differentiate Milia from Other Skin Conditions
1. Acne
Causes:
- Acne is primarily caused by excess oil production, clogged hair follicles, and the growth of bacteria on the skin.
- Hormonal changes, genetics, and certain medications can also contribute to acne development.
Symptoms:
- Acne presents as a variety of lesions, including blackheads, whiteheads, papules, pustules, nodules, and cysts.
- It often causes inflammation, redness, and tenderness.
- Acne can occur on the face, neck, chest, back, and shoulders.
Distinguishing Features:
- Milia are small, firm, and usually white or yellowish in colour, whereas acne can have a range of appearances.
- Unlike acne, it is not inflamed or painful.
- Milia do not have a central opening like whiteheads or blackheads in acne.
2. Whiteheads
Causes:
- Whiteheads, a type of acne lesion, result from clogged hair follicles filled with sebum and dead skin cells.
- Bacterial overgrowth can contribute to the formation of whiteheads.
Symptoms:
- Whiteheads are small, raised, white or flesh-coloured bumps.
- They often have a white or yellowish tip.
Distinguishing Features:
- Milia and whiteheads may appear similar at first glance, both being white and small.
- However, whiteheads are a type of acne and may be surrounded by redness.
- Milia are not associated with inflammation or redness.
3. Sebaceous Hyperplasia
Causes:
- Sebaceous hyperplasia occurs when the sebaceous (oil) glands enlarge and produce excess oil.
- Sun exposure is a known contributing factor.
Symptoms:
- Sebaceous hyperplasia appears as small, flesh-coloured or yellowish bumps.
- These bumps may have a central depression or a tiny hair follicle in the centre.
Distinguishing Features:
- Milia are often mistaken for sebaceous hyperplasia because both can be flesh-coloured.
- However, sebaceous hyperplasia lesions are typically larger and have a central pit or a hair follicle visible.
- Milia are generally smaller and lack these characteristics.
Skin Care Routine for Milia-Prone Skin
Achieving clear and milia-free skin requires a dedicated skincare regimen that focuses on gentle exfoliation, hydration, and the use of specific ingredients. Here’s a step-by-step guide to help you get started:
1. Gentle Cleansing
The foundation of any skincare routine is proper cleansing. it’s essential to choose a gentle, sulphate- free cleanser that won’t strip your skin of its natural oils. Look for cleansers with the following qualities:
- Hypoallergenic: Opt for cleansers that are less likely to cause irritation or allergies.
- Non-comedogenic: These cleansers won’t clog your pores, which is crucial for milia-prone skin.
- Sulfate-free: Sulfates can be harsh on the skin, so avoid them in your cleanser.
Recommended Products:
- Cetaphil Gentle Skin Cleanser
- Vanicream Gentle Facial Cleanser
2. Exfoliation
Exfoliation is a critical step in your skincare routine to prevent milia from forming. Regular exfoliation helps remove dead skin cells that can trap keratin beneath the surface. However, it’s essential to choose the right exfoliator:
- Avoid Harsh Scrubs: Physical scrubs with rough particles can damage the skin and worsen milia. Instead, opt for chemical exfoliants.
- Glycolic Acid: This alpha hydroxy acid (AHA) is excellent for gentle exfoliation and can help prevent it.
- Salicylic Acid: A beta hydroxy acid (BHA) that can penetrate oil, salicylic acid is effective for keeping pores clear.
Recommended Products:
- The Ordinary Glycolic Acid 7% Toning Solution.
- Paula’s Choice Skin Perfecting 2% BHA Liquid Exfoliant.
3. Moisturisation
Hydration is crucial for all skin types, including milia-prone skin. A lightweight, non-comedogenic moisturiser helps maintain your skin’s moisture balance without clogging pores. Look for products that contain:
- Hyaluronic Acid: This hydrating powerhouse can hold 1000 times its weight in water, keeping your skin plump and hydrated.
- Ceramides: These lipid molecules help strengthen the skin’s barrier, preventing moisture loss.
- Glycerin: A humectant that attracts and retains moisture in the skin.
Recommended Products:
- Neutrogena Hydro Boost Water Gel
- CeraVe Facial Moisturising Lotion PM
4. Sunscreen: Your Skin’s Best Friend
Sunscreen is non-negotiable, especially for milia-prone skin. Sun damage can thicken the skin and exacerbate milia. Opt for a broad-spectrum sunscreen with SPF 30 or higher and make it a daily habit.
Recommended Products:
- EltaMD UV Clear Broad-Spectrum SPF 46
- La Roche-Posay Anthelios Melt-in Milk Sunscreen SPF 100
5. Targeted Treatments
In addition to your basic skincare routine, consider adding targeted treatments to address directly. These products often contain ingredients that help exfoliate and break down the keratin trapped beneath the skin’s surface.
Recommended Products:
- Retinoids: Over-the-counter retinol or prescription-strength retinoids can promote cell turnover and prevent it.
- Alpha Hydroxy Acids (AHAs): AHAs like glycolic acid can further assist in gentle exfoliation.
- Serums: Serums with ingredients like niacinamide can help regulate sebum production, reducing the likelihood of clogged pores.
6. Avoiding Comedogenic Products
Comedogenic products are the arch-nemesis of clear skin. Here’s how to dodge them effectively:
- Check Product Labels: Before purchasing skincare or makeup products, scrutinize the ingredient list for comedogenic ingredients like lanolin, cocoa butter, and isopropyl myristate. Steer clear of these troublemakers!
- Patch Testing: Introduce new products cautiously. Conduct a patch test on a small area of your skin to ensure it doesn’t trigger milia formation or irritate your skin.
- Oil-Free Formulas: Opt for oil-free or non-comedogenic formulations. These products are less likely to clog your pores, reducing the risk of milia.
When Should I See My Healthcare Provider?
While most milia are harmless and can be managed with proper skincare, there are situations where consulting a healthcare provider is necessary:
1. Persistent Milia
If you have milia that don’t seem to go away despite your best efforts at home treatment, it’s time to see a healthcare provider. They can assess the situation and recommend appropriate treatment options.
2. Milia En Plaque
As mentioned earlier, milia en plaque that typically requires medical attention. If you notice inflamed, clustered patches on your skin, consult a healthcare provider promptly.
3. Changes in Appearance
Any sudden changes in the appearance of your milia should be a cause for concern. If they become painful, red, or appear infected, don’t hesitate to seek professional advice.
4. Underlying Skin Conditions
If you have an underlying skin condition, such as rosacea or eczema, it’s essential to consult with a dermatologist. These conditions can complicate milia management.
5. Cosmetic Removal
In some cases, it may need to be removed by a healthcare provider. Attempting to remove them at home can lead to scarring and infection. Your provider can perform safe extraction procedures.
Emotional Impact of Milia
It may be small, but their impact on one’s emotional well-being can be substantial. Let’s explore how these seemingly innocuous skin bumps can take a toll on a person’s self-esteem and confidence.
Concealing
Individuals often find themselves spending considerable time and effort trying to conceal these tiny cysts with makeup. The constant need to cover them up can erode self-confidence, making individuals feel self-conscious about their appearance.
Social Withdrawal
In some cases, the emotional impact goes beyond cosmetic concerns. People with severe condition may withdraw from social activities, avoiding gatherings or events where their skin condition might become a topic of discussion or ridicule.
Anxiety and Depression
The emotional toll can extend to anxiety and depression. The constant worry about one’s appearance and the frustration of dealing with an ongoing skin issue can lead to significant psychological distress.
Future Research on Milia
The realm of dermatology is continually evolving. Researchers are actively exploring new avenues to better understand and manage this skin condition. Here are some promising areas of future research:
Genetic Factors
Scientists are investigating whether there is a genetic predisposition. Understanding the role of genetics could lead to more targeted treatments and prevention strategies.
Advanced Treatment Options
Innovations in skincare and dermatology are paving the way for advanced treatments. Researchers are exploring the use of lasers, micro needling, and topical medications to address it more effectively.
Nutritional Interventions
As we mentioned earlier, diet and nutrition may play a role in Milia formation. Future research may uncover specific dietary guidelines to help prevent or manage this condition.
Psychological Support
The emotional impact of Milia is an area that deserves further attention. Researchers are working on developing support programs and therapies to help individuals cope with the psychological toll of this skin condition
Conclusion:
Milia skin may be a common and harmless skin condition, but it can be frustrating to deal with. Understanding the causes, treatment options, and prevention strategies is essential for keeping your skin clear and healthy. Learning how to differentiate milia from other skin conditions like acne, whiteheads, and sebaceous hyperplasia can save you from unnecessary worry and help you seek the right treatment promptly. it may be small, but their impact on an individual’s life can be significant, both emotionally and psychologically.The future research holds promise, with ongoing studies exploring genetics, advanced treatment options, nutritional interventions, and psychological support.
Remember, gentle care, proper skincare, and professional guidance . So, embrace your newfound knowledge, take good care of your skin, and say goodbye to those pearly white bumps for good!
Affiliate disclosure
Kindly take notice that this post may includes hyperlinks that qualify as affiliate links. As a result, I may become eligible to receive a modest commission, without any expense to you, in the event of a purchase made through these hyperlinks featured on this website.Cosmeticknowledge.com is a participant in the Amazon Services LLC Associates Program
https://www.youtube.com/channel/UCwivHo24VuhS0Lj54pzGScA
https://www.facebook.com/profile.php?id=100093483188011
FAQs
Can I pop milia at home like pimples?
It’s best to avoid attempting to pop milia at home. Unlike pimples, it don’t have a pore or opening at the top, making them resistant to popping. Trying to do so can lead to infection or scarring. If you want them removed, consult a dermatologist for safe extraction.
Will changing my diet help prevent milia?
There’s no direct link between diet and milia. However, maintaining a balanced diet and staying hydrated can contribute to overall skin health.
Are there any natural remedies for milia?
While natural remedies like honey or aloe vera may offer some relief, they are not proven treatments. It’s best to consult a dermatologist for effective solutions.
How long will it take to see results with this skincare regimen?
Results may vary, but with consistent use of these products, you can expect to see improvement in a few weeks to a couple of months.
Are there any lifestyle changes I should make to prevent it?
Avoid using heavy, occlusive skincare products and protect your skin from excessive sun exposure.
Can I use these products if I have sensitive skin?
Yes, many of the recommended products are suitable for sensitive skin, but it’s always a good idea to patch-test first.
Can milia turn into acne?
No, it do not transform into acne. They are distinct skin conditions with different causes and characteristics.
Can you pop milia like you do with pimples?
It is not advisable to try and pop it at home. Unlike pimples, it do not have a central opening, and attempting to pop them can lead to infection or scarring. Consult a dermatologist for safe removal.
Are milia the same as acne?
No, they are not the same as acne. While both can appear as small bumps on the skin, they are tiny cysts filled with keratin, not sebum like acne. They are usually white or flesh-colored and do not have the redness or inflammation associated with acne.
Are there any over-the-counter products that can help with Milia?
Over-the-counter products may help with mild cases of Milia by promoting exfoliation and cell turnover. However, for more severe or persistent cases, it’s advisable to seek professional treatment.
Do Milia go away on their own?
In some cases, it may resolve on their own over time. However, it can take several months or even years. If you’re concerned, it’s best to consult a dermatologist for guidance.
Are these skin bumps contagious or can they be spread to others?
No, these skin bumps are not contagious and cannot be spread to others through physical contact or proximity.
Can skin bumps be itchy or cause discomfort?
Skin bumps are typically not associated with itching or discomfort. If you experience itching or discomfort, it’s essential to consult a dermatologist to rule out other skin conditions.